For almost a decade and a half, as an Associate Director of the Johns Hopkins Urban Health Institute, it has been my responsibility to work on one of the most challenging problems in healthcare − improving population health. My work has taken me from the so-called “ivory tower” of Johns Hopkins to the homes, alleys and communities of inner city East Baltimore.
Through my experiences, I’ve realized that despite the U.S. having an amazing healthcare system, it was doing little to reduce the endless flow of patients coming into emergency rooms and hospitals for care. We could treat many physical and psychological ailments, but we were often powerless to provide the support patients and families needed to manage their chronic diseases or truly live “well”.
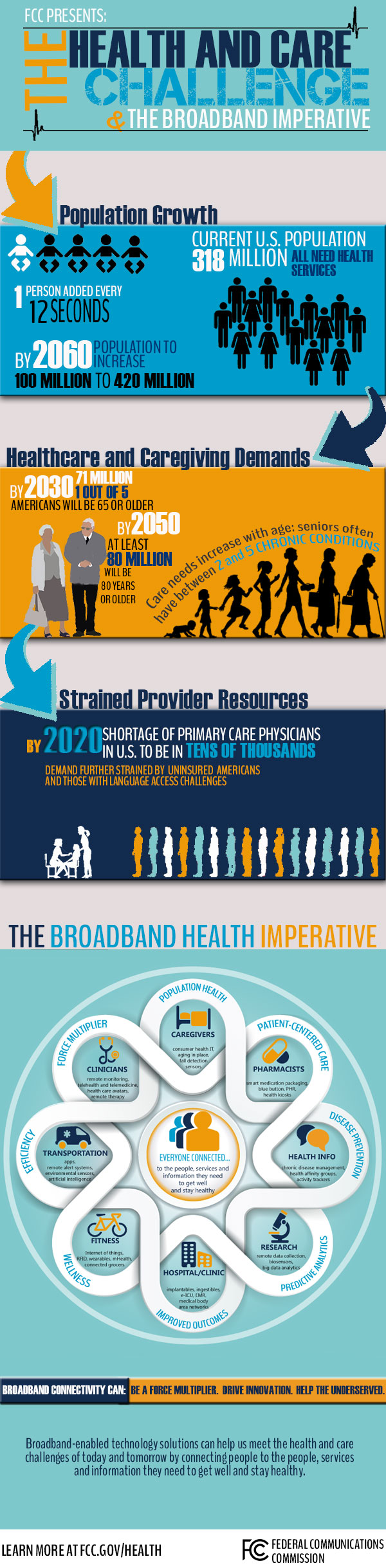
We were powerless not because we could not see what was needed nor because we did not care; rather, as the infographic below suggests, there were too many people that needed treatment and not enough providers to meet their needs. We were taught as medical students to focus on tests, diagnostics, therapies and treatments. I, like many others, believed that if we could just give the best care to every patient, we would ultimately fix our nation’s health care problems. But it isn’t that simple.
Consumers rely on many resources for their health – doctors, social services, nutritionists, pharmacies, caregivers and others. When these “providers” remain unconnected, it is a prescription for frustration, burnout, high costs and suboptimal outcomes.
I am often asked, “Why would a Hopkins doctor come to the FCC?” My answer is simple. It’s because I can’t see how we are going to improve our nation’s health without aggressively pursuing the potential that broadband and broadband-enabled health technologies have to offer. Many of these broadband benefits are already on the horizon. So what better place to be than the FCC!
Recently, U.S. News and World Report looked at how eICUs remove distance from the equation; Forbes tackled the benefits of broadband-enabled telemedicine especially for small businesses; and an October 2014 article in Population Health Management concluded that remote monitoring of congestive heart failure patients reduced readmissions by 38 to 44 percent and produced a return on investment of $3.30 on the dollar – a potential boon for elderly patients with heart conditions.
Hopefully, someday soon, consumers will be able to access any health product or service at any time, day or night. They no longer will be limited by distance, time or place, but only by the speed of their broadband connections. To put it simply, the potential of broadband is enormous for health and healthcare. I am convinced the potential goes far beyond health apps, mHealth, Electronic Health Records, and even big data. The true power of broadband in health will be realized when every consumer is connected, in real time, to the providers, information, support and services they need to get well and stay healthy.
Achieving this goal will not be easy; nor can the FCC do it alone. In the coming months, the Connect2HealthFCC Task force (connect2health@fcc.gov) will continue to work with other policymakers, businesses, organizations, healthcare providers, communications companies and consumers that are interested in this population health vision. We want to hear from individuals—young and old—who are using broadband-based technologies to successfully address health concerns. We want to better understand adoption barriers to broadband-enabled health technologies, experienced by rich and poor alike, and in rural and urban areas. And, we plan to do our part to identify policy and regulatory challenges that inhibit innovation, investment and entrepreneurship in digital health. Our goal is to be a catalyst for making this new broadband-enabled health and care ecosystem a reality.